Why back pain shows up after waking
It can be confusing when your back feels mostly “fine” in the night, yet the first sit-up or bend toward the sink in the morning brings a dull ache—or a sharper catch that wasn’t there before. That mismatch often comes from how still your spine has been for hours, not from anything you did wrong the moment you stood up.
During sleep, low movement means joints and the small stabilizing muscles around the spine tend to stiffen. At the same time, spinal discs can take on more fluid overnight and become slightly fuller. When you first get upright, those fuller discs and stiffer tissues may handle compression and twisting differently than they do later in the day, so normal movements like tying shoes can feel disproportionately intense.
A few minutes of walking or a hot shower may ease it, while reaching, rolling, or bending forward too soon can bring it right back. That “warms up, then settles” pattern can be a clue that the discomfort is linked to overnight loading and tissue behavior rather than a constant, all-day pain signal.
What drives stiffness during overnight immobility
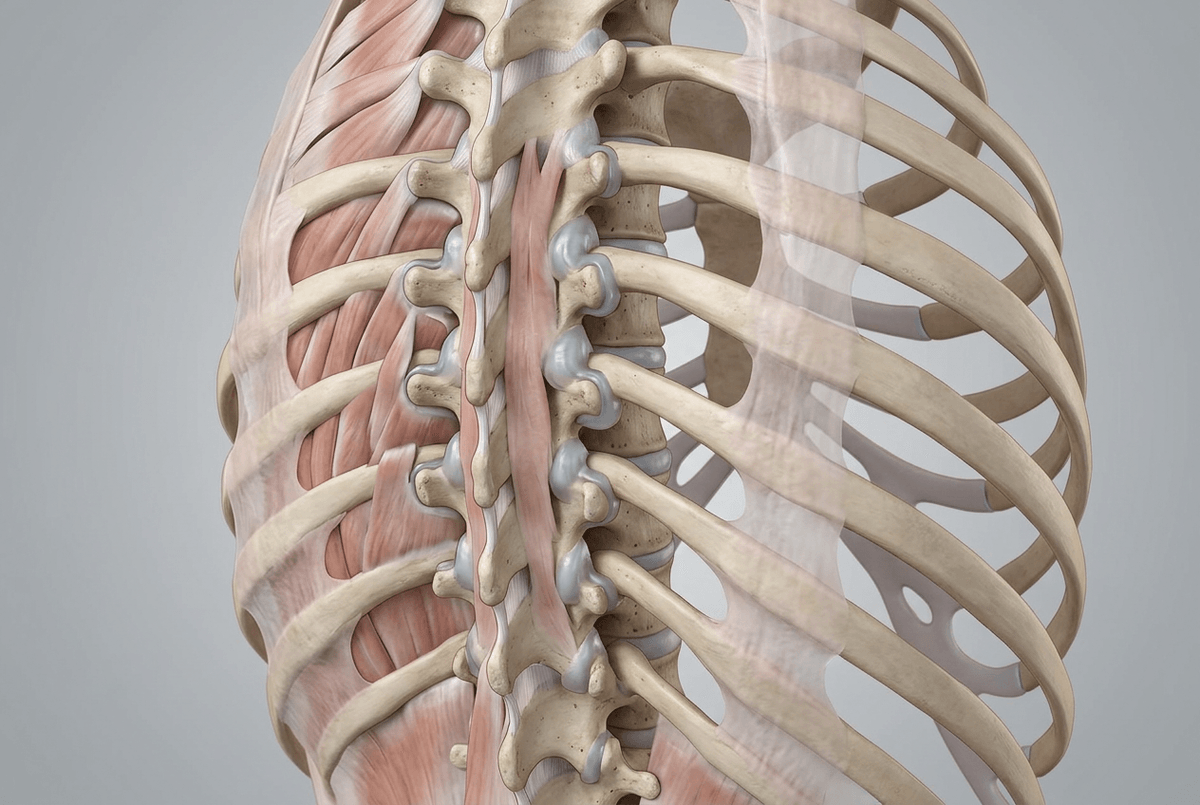
You might notice it most when you try to roll to the edge of the bed and your mid-back feels oddly “stuck,” like the movement takes extra effort. It can be confusing because nothing dramatic happened overnight—yet the first few motions feel tighter than they did before sleep.
One reason is that tissues that usually glide with frequent small movements get fewer “reminders” to do that. When you stay in one position for hours, the joint capsules and nearby connective tissue can hold onto fluid, and the muscles that normally make tiny adjustments don’t cycle on and off as much. By morning, that can translate into a protective, braced feeling—less about damage and more about reduced motion and a nervous system that’s temporarily cautious when you ask for bending or rotation.
At the same time, spinal discs tend to be a bit more hydrated after lying down, which can make them slightly fuller. That fullness can change how pressure is distributed when you first sit, stand, or hinge forward, so a movement that feels routine later in the day may feel sharper or more “pinchy” right after waking—especially if you twist while bent.
Sleep posture and mattress loads certain tissues
You may only notice it when you wake on your stomach or half-twisted, and your lower back feels compressed before you even sit up. Other mornings, you sleep “fine,” but the first reach for the nightstand brings a tight, one-sided pull. That inconsistency often comes down to which tissues were carrying the load for hours—and whether the mattress let you settle into that load or kept you hovering against it.
A mattress that lets your hips sink more than your ribcage can leave the lumbar spine slightly arched for a long stretch of time. In that position, the small joints at the back of the spine and the surrounding muscles may stay shortened and “on,” so they don’t relax in the way they might during a more neutral posture. On the other side, a very firm surface can concentrate pressure at the pelvis and shoulders, nudging the spine into a subtle side-bend or rotation that you might not feel until you try to straighten up.
The same position can be tolerated one night and not the next. If your discs are a bit fuller in the morning, and you start your first movements with a bend-and-twist (even a small one), that combination can make the back read the load as more threatening than it would later in the day—so the “catch” shows up before your body has had a chance to redistribute pressure through easy movement.
Inflammation and sensitized nerves amplify morning signals
Some mornings, the ache doesn’t just feel stiff—it feels “loud,” like a normal movement is being graded as a bigger problem than it should be. That can be especially unsettling when the soreness is more spread out, more tender to touch, or paired with a vague sense that your back is irritated before you’ve really done anything.
In some cases, that extra intensity is less about the posture itself and more about the tissue state you wake up in. Mild inflammation in joints, discs, or surrounding connective tissue can lower the threshold for discomfort, so pressure and stretch register earlier. After hours of stillness, fluid can also pool a bit in these tissues, which may increase swelling and chemical signals that make nearby nerve endings more reactive than usual.
When nerves are sensitized, the nervous system tends to “turn up the gain” on input that would normally be background noise—like the first hinge forward to pull on socks. That’s why a hot shower or a few minutes of walking may help quickly on one day (as circulation and movement change the signal), yet on another day the same motions feel inconsistent or too sharp until the irritation settles down.
When “helpful” stretching makes pain feel worse
You might try to “fix it” the way you’ve always heard—bend forward, tug your knees to your chest, twist side to side—and instead of loosening up, your back feels more guarded or gives a sharper protest. That can feel like a warning that something is seriously wrong, when it may simply be the wrong kind of input for the way your tissues behave first thing in the morning.
After a night of low movement, the spine can be stiffer at the joints while the discs are a bit fuller with fluid. Deep end-range stretching—especially flexion with a little rotation—can briefly raise pressure inside a disc and add shear across small joints that are still “cold.” If nearby nerve endings are already more reactive, that extra pressure can be interpreted as threat, and the nervous system often responds by increasing muscle tone, making you feel tighter right after you stretched.
What adds to the confusion is that the stretch might feel good for a few seconds, then the ache flares when you stand up or take the next few steps. In some cases, it’s not that stretching is “bad,” but that early, aggressive range of motion asks for tolerance that your back hasn’t regained yet that morning.
What tends to ease pain without flaring it
The first few minutes out of bed can feel like your back is negotiating: it wants movement, but not too much, too soon. When the discomfort eases with a slow walk to the kitchen or a warm shower, that’s often your clue that gentle motion is changing the signal without challenging the stiffest, most sensitive ranges right away.
Small, repeated movements tend to work differently than long holds. Brief, low-effort shifts—standing tall, taking a few easy steps, or lightly moving the hips and ribcage through a comfortable range—can help joints and connective tissue redistribute fluid and reduce that “stuck” sensation. At the same time, as circulation increases and muscles cycle on and off, the nervous system may lower its protective guard because the input is consistent and not threatening.
“More” doesn’t always mean “better” in the first 10–60 minutes. If bending forward, twisting, or loading one side brings back the catch, it may help to treat that as information about which positions your back isn’t tolerating yet that morning, rather than a sign that you’re doing nothing right.
Signals that suggest something beyond routine stiffness
Some mornings, it doesn’t “unlock” the way you expect. Instead of easing as you walk around, the pain may stay sharp, intensify, or feel more precise—like a single spot that bites with each step. That mismatch can be unsettling because it breaks the usual pattern of stiffness that loosens once tissues warm and fluid shifts.
Signals that tend to fit less with routine morning stiffness include pain that doesn’t change after an hour or two of normal movement, pain that repeatedly wakes you from sleep, or symptoms that spread beyond the back (like persistent tingling, numbness, or weakness in a leg). Another flag is trouble controlling bowel or bladder function, which isn’t typical “disc fullness” discomfort and may need urgent attention.
It can also be worth a closer look if a fever, unexplained weight loss, a recent fall, or pain that feels constant in any position shows up alongside your back symptoms. If you’re unsure, choosing a same-day call to a clinician can be a reasonable next step—especially when the pattern is new, escalating, or simply not behaving like it usually does.