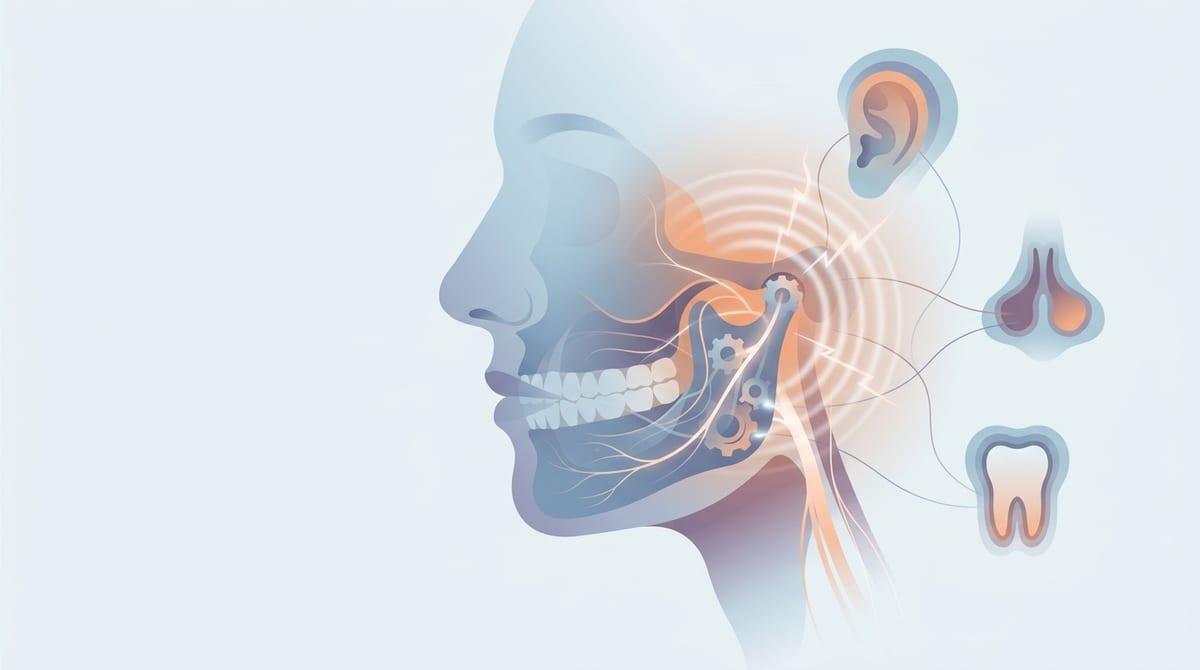
Why jaw pain can imitate other conditions
A vague heaviness near the hinge in front of the ear is often where it shows up first. Then, without much warning, it can shift—starting to feel more like a tooth problem, a sinus issue, or even pressure deep in the ear. That kind of confusion isn’t unusual. The lower face is a crowded area, where jaw muscles, teeth, joint tissues, and nearby spaces all sit close together—and they’re all involved in everyday actions like chewing, talking, yawning, or even clenching your teeth during sleep.
What makes it harder to pinpoint is how these areas share nerve pathways. Signals from different parts of the jaw and face travel along overlapping routes, so the brain can sometimes “misread” where the irritation is coming from. A sore chewing muscle might feel like a deep toothache, while joint irritation can come across as ear discomfort—especially when the sensation shifts with movement.
Even so, certain patterns can still offer useful clues. A dull, spreading ache after heavy use often points toward muscle strain. In contrast, sharper, more localized pain that lingers may behave more like a dental or nerve-related issue. And if the pain becomes intense, swelling appears, a fever develops, or your bite suddenly feels different, it’s usually a good idea to have it checked rather than trying to figure it out on your own.
Clenching and grinding overload the chewing muscles

You might notice it most when you first wake up: the jaw feels heavy, the cheeks feel tired, and opening wide takes a little extra effort. The discomfort can be uneven—worse on one side, better by midday, then back again after a tense commute or a long stretch of screen time—making it easy to misread as a “bad tooth” or a random ear issue.
Clenching and grinding load the chewing muscles in a way they aren’t meant to handle for long. Muscles like the masseter and temporalis can stay partly contracted for minutes to hours during sleep or concentration, which limits normal blood flow and keeps the tissue working in a low-oxygen state. Over time, that can leave the muscle irritable and chemically “noisy,” so everyday chewing or talking feels like it’s pushing on a bruise. Because these muscles attach near the temple and along the lower jaw, the ache may spread into headache patterns or create a vague sensitivity that doesn’t match one specific tooth.
What adds to the confusion is how automatic it can be. Many people don’t realize they’re clenching until they catch themselves with teeth touching at rest, or they notice morning soreness without any clear daytime trigger. In some cases, the nervous system starts to anticipate pain, and the jaw tightens protectively—an effortful loop that can keep the muscles tender even when you’re trying to “relax.”
Temporomandibular joint irritation changes bite mechanics
Sometimes the first thing you notice isn’t pain at all—it’s that your teeth don’t seem to meet the same way for a moment, or the jaw tracks slightly off when you take a bite. It can feel inconsistent: fine at lunch, then “wrong” again after a long phone call or a wide yawn, which makes it hard to trust what’s actually going on.
When the temporomandibular joint is irritated, the problem may be less about the teeth and more about how the joint is guiding the jaw. The joint is a hinge-and-slide system with a small cartilage disc that helps the movement stay smooth. If the tissues around it are inflamed or the disc isn’t gliding cleanly, the jaw may shift to a path of less resistance. That subtle detour can change which teeth touch first, concentrate pressure on one side, and make chewing feel awkward—even if the teeth themselves are healthy.
Clicks or pops can show up in this phase, but not everyone gets them, and a click doesn’t always match the level of soreness. The uncertainty can lead to extra “testing” bites and frequent repositioning, which keeps loading the joint and can make the bite feel even more variable. If the change in bite persists or you can’t open normally, it’s usually worth getting assessed in person rather than waiting it out.
Dental and nerve pain that masquerades as jaw ache

It’s often a small, nagging detail that stands out first: one spot feels “off” when something cold hits it, or there’s a twinge when you bite down that disappears as soon as you stop chewing. The sensation can still land in the jawline or near the joint, which is unsettling because it doesn’t behave like a single sore muscle you can predict.
In some cases, pain that seems like it’s in the jaw is coming from a tooth or the tissues around it. The trigeminal nerve carries signals from both the teeth and the jaw area, and the brain doesn’t always map those signals cleanly—especially when they’re coming from deeper structures like the tooth pulp. That’s why a cracked tooth, an irritated filling, or gum inflammation can read as a dull jaw ache until a specific trigger (pressure, temperature, sweetness) makes it feel more clearly “tooth-based.”
Nerve-type pain can add another layer of confusion. Instead of a steady ache, it may feel sharp, brief, or electric—then vanish, leaving you unsure whether it was real or just a fluke. Because those zaps can be set off by talking, brushing, or a light touch to the face, people sometimes assume it’s the joint “catching,” when the pattern may fit better with a sensitized nerve pathway than with bite mechanics.
Referred pain from neck, ear, or sinuses
It can be strange when the jaw feels sore, but the most noticeable pressure sits “inside” the ear, or the ache seems to climb up toward the temple and down into the neck. The location may even swap from day to day, which makes it hard to decide whether you’re dealing with a jaw problem or something happening nearby.
Part of that mismatch can come from referral—when irritated tissue in one area is felt somewhere else. The jaw, ear canal region, upper throat, and parts of the neck share overlapping nerve input, and the brain can have trouble separating those signals when they arrive together. If the neck muscles are tight, for example, they can pull on head-and-jaw positioning and keep the chewing muscles working harder than usual, so the “jaw pain” can be driven as much by posture and muscle guarding as by the joint itself.
Sinus and ear inflammation can muddy the picture further. Congestion or Eustachian tube irritation may create a full, pressurized sensation that’s easy to mistake for TMJ trouble—especially if chewing or yawning briefly changes that pressure. The jaw can feel involved because it’s moving near the irritated area, even when the primary trigger isn’t coming from a tooth or the joint.
What drives pain flare cycles beneath the surface
A flare can sneak up after a day that didn’t seem unusual—then by evening the jaw feels “hot,” chewing feels harder, and even light contact between the teeth starts to feel like too much. What makes it confusing is the delay: the trigger might have been hours earlier, and the soreness doesn’t always match how much you used your jaw in the moment.
One thing that can drive this is sensitization, where irritated tissues and nearby nerve pathways become easier to activate. After repeated loading, the joint lining and chewing muscles may release inflammatory chemicals, and the trigeminal nerve can start firing with less provocation. At that point, normal movement can feel threatening, so the jaw reflexively guards—muscles tighten to “protect,” blood flow drops, and the tissues stay chemically irritated. The person often interprets this as a new injury, when it may be the same loop running louder.
Sleep and attention can make the cycle feel inconsistent. Light, fragmented sleep can raise pain sensitivity the next day, and stress can pull the jaw into a semi-clenched position without noticing. Then a click, a twinge, or a “wrong bite” moment becomes something you monitor repeatedly, and that extra checking can keep loading the system even when you’re trying to figure it out.
Treatment options that fit the most likely cause
At some point the question stops being “what is this?” and becomes “what actually changes it?” That’s where treatment can feel oddly uneven: the same ache may calm down with a few days of reduced jaw loading, or it may stay stubborn until a specific tooth, sinus issue, or nerve pathway is addressed. The uncertainty is part of the signal—different tissues respond to different kinds of help.
When the pattern looks muscle-driven (morning heaviness, soreness that builds with chewing, tenderness along the cheeks or temples), first-line care is often aimed at lowering the workload and letting blood flow and muscle chemistry normalize again. In contrast, when the joint feels mechanically involved (variable bite, catching, limited opening), the focus is usually on reducing irritation inside the joint and avoiding repeated “testing” movements that keep the lining inflamed.
If symptoms behave like dental disease or nerve irritation—sharp pain with temperature or biting, swelling, persistent one-sided throbbing, or electric zaps—muscle or TMJ strategies may not touch the source. That’s a place where an in-person dental or medical exam matters sooner rather than later, especially if fever, facial swelling, drainage, or rapidly worsening pain shows up.