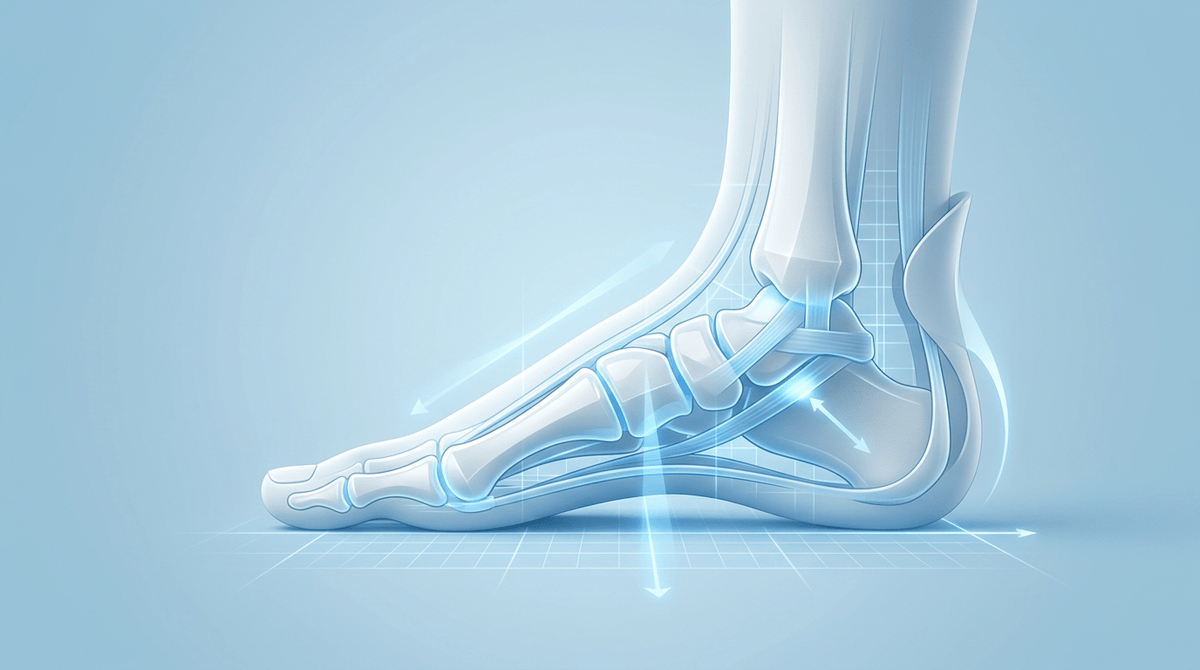
First question: sprain or something more serious?
It’s often the second attempt to move that feels most confusing—when the first jolt fades, but the joint still won’t do what you expect. You might be able to take a few steps or pick up a cup, yet a specific angle sends a sharp warning. That mismatch can make it tempting to label it “just a sprain” or, on the other hand, assume the worst based on how much it hurts.
Early on, pain alone isn’t a reliable grader. A stretched ligament can hurt intensely because the joint lining and nearby tissues are rich in pain sensors, and swelling increases pressure in a tight space. A small fracture can sometimes feel oddly manageable at rest, then spike with loading or gripping because force is traveling through a disrupted area.
What tends to separate “sprain-like” behavior from something that deserves more caution is how the joint performs: whether you can bear weight through the ankle for several steps, or use the wrist for gentle pushing without a deep, pinpoint pain over a bone. Instability—feeling like it wants to give way—can be a different signal than soreness, even when bruising looks dramatic.
What actually gets injured in wrist and ankle
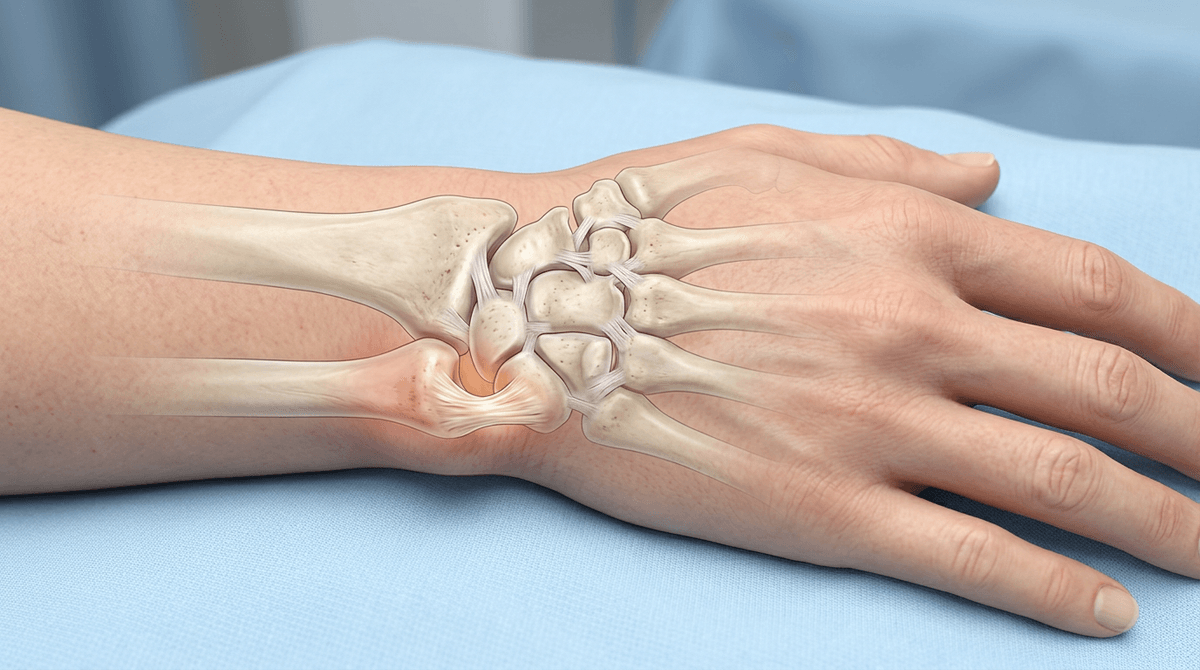
Sometimes the swelling makes everything feel “generally angry,” but the tissue that actually took the hit is usually more specific. In an ankle twist, the most common injury is to the outer (lateral) ligaments that resist the foot rolling inward—often the anterior talofibular ligament first, then deeper structures if the force was bigger. With a fall onto an outstretched hand, the wrist can strain small stabilizing ligaments between the carpal bones, or irritate the triangular fibrocartilage complex (TFCC) on the pinky-side—both of which can make rotation and gripping feel unexpectedly limited.
That detail matters because ligaments behave differently than muscle: they’re designed for stability, so when fibers overstretch or tear, the brain often “turns down” movement as a protective reflex. The joint may feel stiff or unreliable not only from swelling, but because the nervous system is treating certain angles as unsafe. That’s also why pain can seem inconsistent—okay in a straight line, sharp with a pivot, push-up motion, or a twist—depending on which stabilizer is being tugged.
Why swelling, bruising, and pain can escalate
A few hours later, the joint can look worse even if you’ve been “careful,” and that can feel like a bad sign. The area may puff up, the skin may feel tight, and the pain may spread from one spot into a wider ache. That escalation is uncomfortable—and it can be inconsistent, where it throbs at rest but bites most when you try a very specific motion.
Part of what’s happening is mechanical. Tiny blood vessels can tear along with ligament fibers, and fluid moves into the tissue spaces. In an ankle or wrist, there isn’t much room to expand, so pressure builds and irritates nearby pain sensors. Bruising often tracks with gravity rather than the exact injury site, which is why a sprained ankle can look purple near the toes later, or a wrist injury can discolor the hand even when the tender point is higher up.
Pain can also ramp up because the nervous system starts guarding. When a joint feels unstable, the brain may tighten surrounding muscles and restrict certain angles automatically. That protective stiffness can make normal movements feel surprisingly sharp, even when the original damage isn’t getting “bigger” moment to moment.
A simple at-home plan that protects healing tissue
The first night is when it often becomes clear what “using it a little” really costs. You might notice that every short walk around the house makes the ankle feel fuller, or that a few routine grips—phone, doorknob, steering wheel—leave the wrist buzzing afterward. That doesn’t automatically mean it’s severe, but it does mean the tissue is still reacting, and the reaction can outpace what you can see.
In the first 24–72 hours, the goal at home is usually to limit the repeated stress that re-triggers swelling while still keeping the joint from going completely “offline.” Light, comfortable movement in a pain-limited range can help fluid move out, but higher-load moments—pushing up from a chair with the wrist, pivoting on the ankle—can keep reopening tiny irritated vessels and keep pressure high. That’s why symptoms can feel inconsistent: okay at rest, worse after small bursts of normal life.
External support often helps mainly by reducing motion at the angles that provoke guarding. A snug elastic wrap or brace can make the joint feel more predictable and may blunt that reflexive muscle tightening, even though it can’t “heal” the ligament directly. If swelling is rapidly increasing, pain is becoming sharply pinpoint over a bone, or function is dropping instead of slowly returning, that’s a different pattern than a typical settling-in phase.
The common mistake: immobilizing too much too long
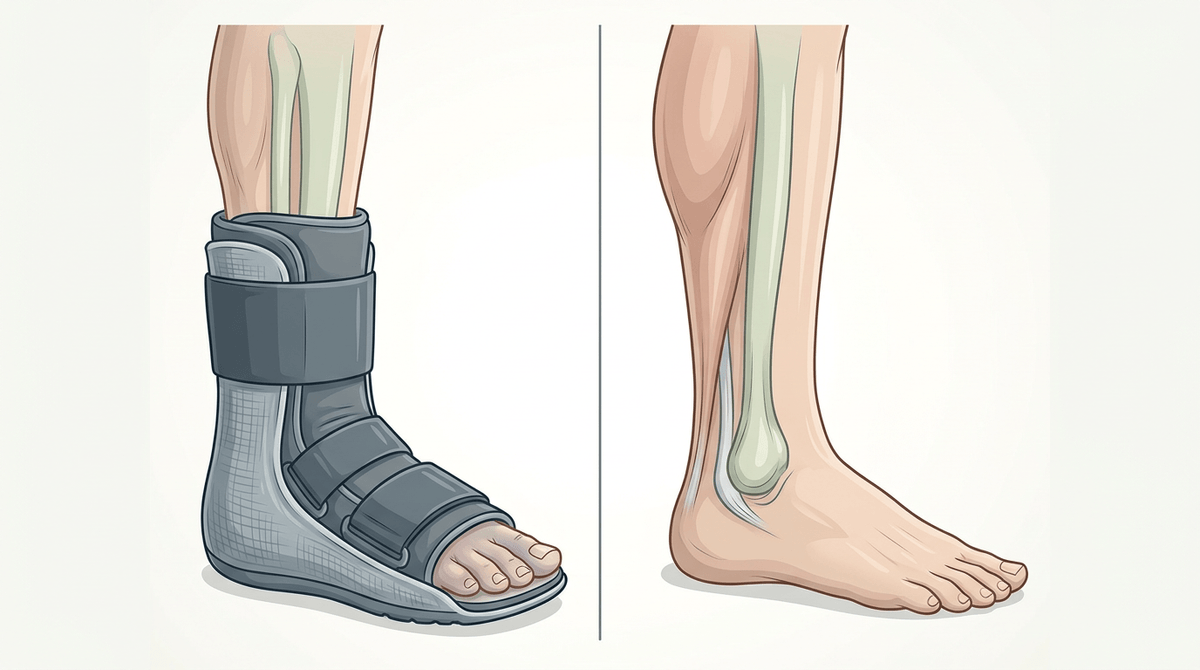
It can feel like a relief when the joint is finally “quiet” inside a stiff brace or splint—less tugging, less surprise pain. The problem is that comfort can be misleading. If you stop moving the wrist or ankle almost entirely for more than a short window, the next time you try to use it, it may feel strangely tight and weak in a way that doesn’t match the original injury.
Part of this is a normal body response to stillness. When a joint isn’t taken through regular, low-effort motion, fluid tends to linger, the capsule and surrounding tissues adapt to a smaller range, and the nervous system keeps the “guarding” setting turned up because it hasn’t gotten safe feedback. Muscles that help stabilize the joint also decondition quickly when they’re not asked to do even small, controlled work.
Over-immobilizing can also blur the signal you’re trying to track. A brace can mask instability or bone-specific pain at first, then those symptoms show up later when you finally load it—sometimes after several days—making it harder to judge whether the injury is actually improving.
Red flags that should trigger same-day evaluation
Sometimes it’s the way the pain “chooses a point” that changes the whole calculation. Instead of a broad ache, you may notice a very specific, sharp tenderness right on a bone—at the wrist near the thumb-side (snuffbox area) or at an ankle bone—where even light pressure feels wrong. That kind of pinpoint pain can be easy to misread as “just sore,” especially if bruising elsewhere looks worse, but it can be a different pattern than a ligament strain.
Function is another tell, even when you’re trying hard to push through. If you cannot take four steps on the injured ankle, cannot bear weight again after a short rest, or your wrist cannot do gentle loading (like pushing up from a chair) without a deep spike, that loss of usable strength matters. A joint that feels like it’s giving way, looks noticeably deformed, or has rapidly expanding swelling can signal more than routine inflammation.
Pay attention to body signals beyond pain. New numbness, tingling, a cold or unusually pale hand/foot, or pain that keeps climbing despite rest and support can suggest pressure or circulation issues. If any of these show up, same-day evaluation is usually the safer move.
If it’s not improving, what clinicians check
After a few days, what gets frustrating is the lack of trend. The swelling may look a little better, but the joint still “catches” at the same angle, or the first steps in the morning feel no easier than they did on day two. That inconsistency is often what brings people in—not maximum pain, but the sense that the tissue isn’t calming down the way they expected.
In a clinic, the first check is usually pattern-based: exactly where the tenderness lives, whether it’s bone-specific, and whether certain motions reproduce a deep, localized pain versus a broader stretch. They’ll compare side to side for laxity and end-feel (how the joint stops), because a high-grade ligament tear can feel mechanically different even if bruising is similar. If the story and exam raise concern for a fracture or an injury that doesn’t show well on basic X-ray, imaging choices may widen, because some structures keep hurting simply because they’re still being loaded in a way they can’t yet tolerate.
They’ll also look for the “quiet” problems that change the plan: reduced circulation, nerve irritation, or a level of swelling that’s maintaining pressure and guarding. If progress is stalled, it’s usually less about proving you were “right” or “wrong” and more about matching the next step to what the joint is actually doing now.